Photosensitivity
People with lupus may develop rash or disease flares from exposure to ultraviolet (UV) radiation from the sun or other sources such as fluorescent bulbs. This reaction is called photosensitivity. UV rays can initiate or worsen symptoms of lupus including rash, sores, fever, arthritis, or fatigue. UV radiation contains UV-A, UV-B and some people with lupus may be more sensitive to one type, while others are sensitive to both types of radiation. It is important to protect yourself from UV exposure to help prevent lupus flares. Visit Skin Self-Care for Lupus to learn ways to reduce UV exposure.
Rash
Rashes are changes in skin color and texture, such as redness and spots. Many people with lupus experience rashes and there is a wide variety of ways the rash can appear. A few of the most common types are described below.
One type of rash called acute cutaneous lupus erythematosus usually affects skin that is exposed to the sun. This includes the butterfly or malar rash that appears over the cheeks and nose. Other common areas include the backs of the hands and fingers (particularly, the skin between the knuckles) and the outside of the forearms. This rash is usually red, may feel warm, slightly swollen or raised, and may involve blisters. The rash may last for hours to weeks before fading.
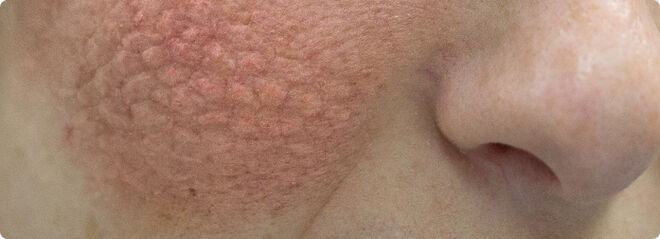
Another type of rash known as subacute cutaneous lupus erythematosus may start as small, red, scaly bumps that may spread to combine to form circular clusters and patches. This rash is usually located over the upper back, upper chest, shoulders, and outside of the forearms. This type of rash usually does not affect the face. Many different drugs can cause this type of rash, including some types of blood pressure lowering medications, cholesterol treatment, non-steroidal anti-inflammatory medications, acid reflux medications and antifungals.
15-30% of people experience another rash called discoid lupus erythematosus which appears as a patch of red skin with a well-outlined border that slowly expands outward at the border with the central skin becoming flattened, scarred and often losing pigment. This rash usually involves the face, neck, scalp, ears, although can occur anywhere on the body. After scarring occurs, the changes may be permanent.
Rashes are often triggered by the sun and may be associated with other lupus symptoms such as joint pain or oral sores. Some rashes cause scarring or changes in skin color, while others do not.
Seeing a Doctor for Rash
Your doctor will determine the cause of your rash by asking you questions about your symptoms and thoroughly examining your skin. They may perform lab tests to measure your lupus activity. You may be referred to a dermatologist. This could include a skin biopsy to rule out other conditions that can cause a rash.
Hair Loss
Hair loss, known as alopecia, may occur in people with lupus. When hair loss occurs with other symptoms of lupus flares (such as rash, joint pain, or oral sores) the hair loss may be driven by lupus activity.
If other symptoms of lupus are not active, it may be that the hair loss is from another cause. A common cause for hair loss is telogen effluvium, which occurs when the body is under psychological or physical stress. Telogen effluvium occurs when more hair follicles than usual are pushed into the shedding (telogen) phase of the hair cycle at once. You might see hair come out when you shower or groom your hair. Hair loss typically occurs two to three months after a major stressor and may continue for six to nine months. Other causes of hair loss include iron deficiency or thyroid problems.
Seeing a Doctor for Hair Loss
Your doctor will determine the cause of your hair loss by asking you questions about your symptoms and examining your scalp. They may perform lab tests to assess lupus activity. Regrowth of hair loss due to lupus may depend on the presence of rash or scarring in the area, so it is helpful to undergo an examination to determine if treatment is needed.
If hair loss is not thought to be due to high lupus activity, in many cases, hair will grow back on its own as you recover from the acute stress within six to nine months. When you see your hair falling out it might contribute to your stress, so it is important to practice relaxation and stress management strategies to break the cycle. Your excessive hair loss will likely end once your stress levels recover.
Other self-care strategies can help you cope with the stress and life disruption that can be caused by lupus' impact on skin and hair. To learn more, visit: